Discovering a lump in the breast can be a source of significant anxiety. It’s crucial to understand that not all breast lumps are cancerous. In fact, a majority of breast lumps are benign, meaning they are non-cancerous and do not pose a life-threatening risk. However, distinguishing between a benign and a malignant (cancerous) lump requires medical evaluation.
This article will walk you through exactly what benign and malignant mean, what common benign conditions look and feel like, and the specific signs that should prompt you to see a doctor without delay.
What Do Benign and Malignant Actually Mean?
Benign means non-cancerous. It consists of normal cells that have formed an unusual cluster. Importantly, these lumps are typically not life-threatening, do not invade nearby tissues, and do not spread to other parts of the body. Think of it like a harmless crowd that gathered in one spot and has no intention of going anywhere.
They have several distinct features:
- Growth: They grow slowly and remain localised to the area where they originated. They do not invade surrounding healthy tissue.
- Encapsulation: They are often well-defined, feel smooth, and can be easily moved within the breast tissue. A capsule of normal tissue may surround them.
- Spread (Metastasis): Benign tumours do not spread to other parts of the body (metastasise).
- Recurrence: While some benign conditions may recur, they are generally not life-threatening.
- Treatment: Often, no treatment is needed beyond monitoring. If they cause discomfort or are very large, they may be surgically removed.
Malignant means cancerous. Malignant cells grow in an uncontrolled way, invade nearby tissue, and have the potential to travel through the bloodstream or lymph nodes to distant organs. This is breast cancer. It requires treatment, and the earlier it is caught, the better the outcomes. Early-stage breast cancer in India now has survival rates comparable to global figures when detected and treated promptly.
Malignant tumours, or breast cancer, are characterised by:
- Growth: Malignant cells multiply rapidly and aggressively, often invading and destroying nearby tissues and structures.
- Boundaries: They are often irregular in shape, feel hard, and may be fixed or firmly attached to the surrounding tissue. They typically have poorly defined borders.
- Spread (Metastasis): This is the most dangerous aspect. Malignant cells can enter the bloodstream or lymphatic system and travel to distant organs, forming new tumours in the bones, lungs, liver, or brain. This is known as metastasis.
- Recurrence: Cancer cells can recur even after treatment.
- Treatment: Requires aggressive treatment, which can include surgery, chemotherapy, radiation therapy, hormone therapy, and targeted therapy.
| Note It is important to know that you cannot tell the difference by touch alone. Neither can your doctor without a scan/biopsy/biomarker tests. What you can do is learn the patterns — and know when to go get checked. Take a breast self examination today. To know how to go about it, click here: https://www.karkinos.in/k-vani/diy-breast-self-examination-bse-step-wise-guide/ |
What Could the Lump Be?
When a lump is discovered, it could be one of several possibilities, both benign and malignant. Only a physician using suitable diagnostic procedures can make a definitive determination.
Potential causes of a breast lump include:
- Cysts: Fluid-filled sacs that are common in women aged 35–50 years, particularly before menopause. They are usually smooth, well-defined, and mobile, and are typically benign.
- Fibroadenomas: The most common solid benign tumours in the breast. They are firm, smooth, rubbery, and easily movable. They are more common in younger women.
- Fat Necrosis: Scar tissue formed after an injury or surgery to the breast. The area may feel firm and irregular.
- Abscess or Infection (Mastitis): A painful, swollen area that often occurs in breastfeeding women but can happen at any time.
- Phyllodes Tumours: These are rare tumours that can be benign, borderline, or malignant.
- Breast Cancer: Malignant growth.
Benign Conditions That Need Medical Examination
While many benign conditions are harmless, it’s essential to understand that any new or unusual breast change requires medical attention to rule out cancer. Furthermore, some benign conditions can increase the future risk of breast cancer or require monitoring.
A medical examination by a licensed doctor, gynaecologist, or oncologist is necessary for any breast lump. However, for creating awareness, the following common benign conditions are listed:
-
- Fibrocystic Changes: This is not a disease but a common condition where the breasts feel lumpy, rope-like, or dense. Symptoms often worsen before a menstrual period. While benign, a clinical breast exam and imaging are needed to confirm the diagnosis and ensure a dominant lump is not cancerous.
- Lipoma: A lipoma is a slow-growing lump of fatty tissue sitting just beneath the skin. In the breast, it feels soft and doughy, almost like a small pillow you can gently press into. It moves easily, has no firm edges, and causes no pain. Lipomas are completely harmless and rarely need any treatment. They tend to stay the same size for years, though some grow slowly over time.
- Intraductal Papillomas: Small, benign, wart-like growths that form in the lining of a milk duct. They may cause nipple discharge, which necessitates medical examination.
- Atypical Ductal Hyperplasia (ADH): ADH is not something you can feel. It is a microscopic finding discovered during a biopsy done for another reason. It means cells inside the milk ducts are growing slightly abnormally, without being cancerous. However, women with ADH have a 4–5 times higher lifetime risk of developing breast cancer compared to the average. If your biopsy report mentions ADH, ask your doctor about an enhanced screening plan and whether genetic counselling is right for you.
| If a lump or any change is noticed in the breast, the first step is to schedule an appointment with a doctor for a clinical breast exam. |
Early detection is key to achieving the best possible outcomes, especially if the lump proves malignant. The next steps after the initial visit might involve scheduling an imaging test, so be prepared for a follow-up appointment. Diagnostic tools such as mammography and ultrasound are used to evaluate a breast lump. If needed, a biopsy is performed to definitively determine its nature. Biomarker tests are typically performed after a cancer diagnosis to guide treatment.
Benign vs Malignant
| Benign (Non-Cancerous) | Malignant (Cancerous) | |
| Feel | Smooth, soft, or rubbery | Hard, irregular edges |
| Movement | Moves freely when pressed | Often fixed, does not move |
| Pain | Often tender, especially before periods | Usually painless (not always) |
| Edges | Well-defined, clear border | Blurry, ill-defined border |
| Growth | Stable or fluctuates with cycle | Grows steadily over weeks |
| Skin changes | Skin looks normal | Dimpling, puckering, redness |
| Nipple | No change | Discharge (especially bloody), inversion |
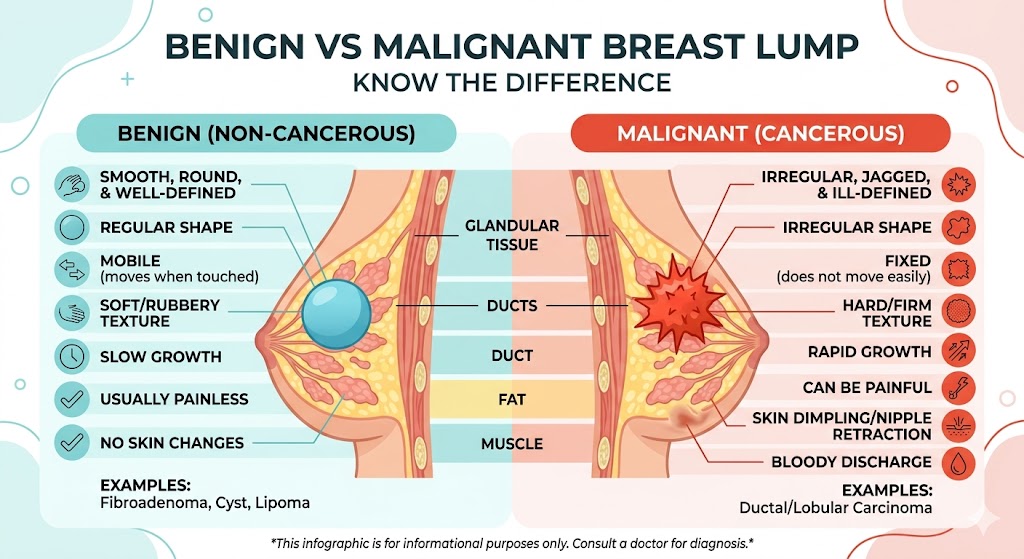
**This image is for informational purposes only. For medical advice or a diagnosis, consult a professional cancer doctor.
When Must You See a Doctor — No Waiting
| See a doctor if you notice any of these:
• A lump that does not go away after your next menstrual period • A lump that is growing — larger week on week • A lump that feels hard and fixed (does not move) • Skin changes: dimpling, puckering, orange-peel texture, or redness • Nipple discharge, especially if it is bloody or comes from one nipple only • Nipple inversion (turning inward) that is new • Any new lump if you are post-menopausal • A swollen lymph node in your armpit alongside a breast change |
In India, many women delay seeking care because of fear, embarrassment, or the belief that a lump “will go away on its own.” Sometimes it does. But when it doesn’t, that delay costs precious time. A 10-minute visit to a general physician, who can refer you for an ultrasound, is all it takes to start ruling things out.
Your Questions, Answered
Q Is every breast lump cancer?
No. The majority of breast lumps, especially in women under 40, are benign. Common causes include fibroadenomas, fibrocystic changes, mastitis, and intraductal papillomas. Finding a lump is a reason to get checked, not a reason to panic.
Q How do I know if my lump is benign or malignant?
You cannot tell for certain by touch alone, and neither can a doctor without an ultrasound or biopsy. Smooth, movable lumps that change with your cycle are more often benign. Hard, fixed lumps that grow steadily need prompt evaluation. The only way to be sure is to get it checked by a doctor.
Q What is a fibroadenoma, and is it dangerous?
A fibroadenoma is the most common benign lump in younger women. It feels like a smooth, rubbery ball that moves easily under your fingers. It is not cancer and does not become cancer in most cases. An ultrasound will confirm the diagnosis.
Q Can a benign condition turn into breast cancer?
Most benign conditions like fibroadenoma, fibrocystic changes, and mastitis carry no increased cancer risk. The key exception is Atypical Ductal Hyperplasia (ADH), found on biopsy, which raises lifetime risk and warrants a closer surveillance plan with your doctor.
Q: When should I see a doctor about a breast lump?
See a doctor if a lump persists beyond your next period, grows, feels hard or is attached to the skin, or if you notice nipple discharge, skin dimpling, or any new lump after menopause.
A doctor’s examination is recommended
Finding a breast lump is frightening. But fear, when it moves you toward care rather than away from it, can be a quiet kind of courage. Most lumps turn out to be nothing to worry about. Most stories end in relief.
So let this be the nudge, not the worry. Get it checked. Ask questions to your healthcare provider. Know that understanding your own body is never wasted, and that early attention, always, opens more doors than it closes.
References
Guray M, Sahin AA. Benign breast diseases: classification, diagnosis, and management. The Oncologist. 2006;11(5):435–449. doi:10.1634/theoncologist.11-5-435
Hartmann LC, Sellers TA, Frost MH, et al. Benign breast disease and the risk of breast cancer. New England Journal of Medicine. 2005;353(3):229–237. doi:10.1056/NEJMoa044383
Karkinos Healthcare
media@karkinos.in
